
When information analysts use data to describe healthcare they usually start with institutions or departments or staff disciplines and measure things within those categories. How many hospital admissions? How many GP consultations? How many A&E attendances? How many district nurse contacts? It's as if we are looking at a map of healthcare where boxes represent buildings (e.g. hospitals or A&E departments) and circles represent staff disciplines (e.g. district nurses or GPs), and we then populate these shapes with aggregated numbers.

But when you ask healthcare managers and clinicians to describe their own worlds—what does healthcare look like to them?—they usually place the patient in the centre of that world and they stress the need to be able to track individual patient journeys across and between the different staging posts of the health and social care system. They are less interested in how many district nurse contacts there were or how many A&E attendances, or how many hospital admissions; they are instead more interested in how many times Patient X saw a district nurse before being seen by their GP, and what happened to them after the GP referred them directly to A&E, and they were subsequently admitted, and so on.
So whilst information analysts have one type of map that they are used to populating with data (the circles and squares are similar to an actual geographical map's countries, cities, towns and districts), managers and clinicians are more interested in a map on which patient journeys are superimposed, in the way Marco Polo's journeys can be drawn over the map of Asia.
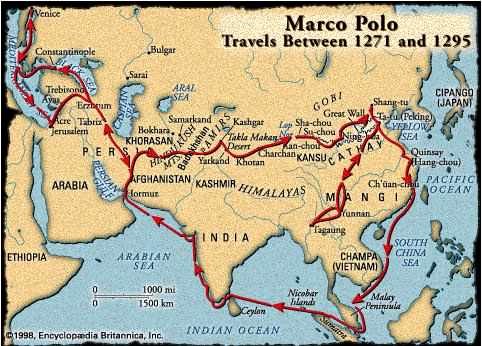
The challenge for NHS information analysts is to square this circle. Can we simultaneously show what the system looks like, as well as also showing what individual journeys within that system look like? And can we show individual journeys in such a way that they still enable managers and clinicians to make useful generalisations about processes that will lead to performance improvement?
[25 July 2017]